- Radiation Oncologist
- Radiotherapy technologists (RTT) / Therapeutic radiographers
- Health Play Specialist
- Dosimetrist and Clinical Physicist
- Anesthesiology Team
- Other health professionals (e.g. nutritionist, physical therapist)
Radiation Oncologist
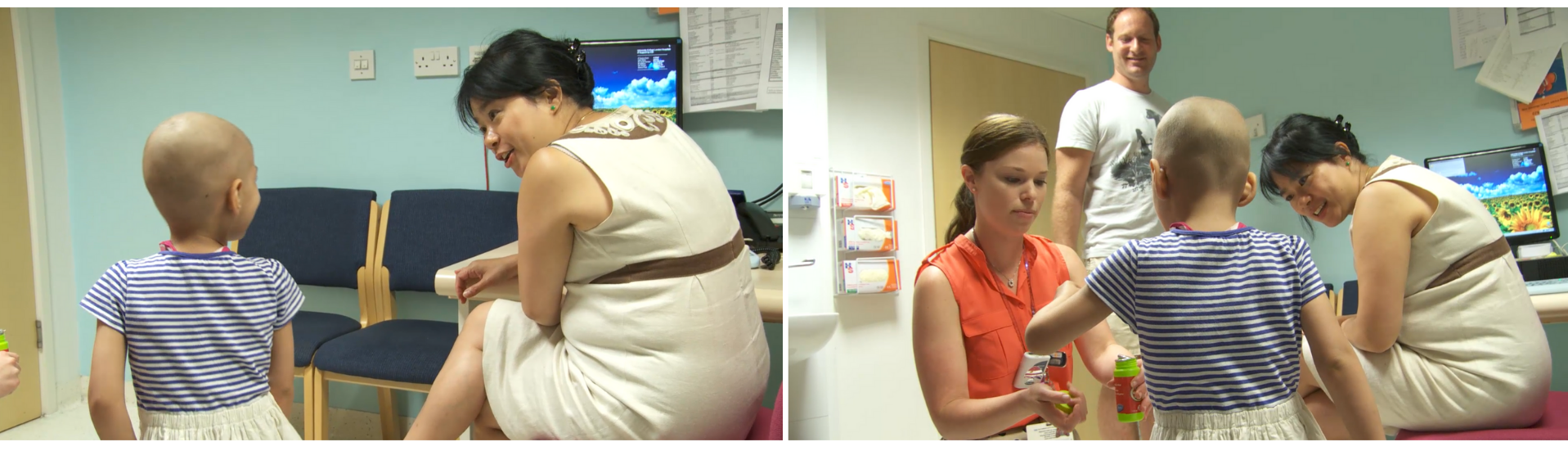
The radiation oncologist or clinical oncologist is the doctor who will plan and oversee the radiation treatment. She or he is part of the paediatric oncological medical team that discusses and monitors the entire treatment programme of a child. During your initial visits to the radiotherapy department, the radiation oncologist will explain the treatment, its value and potential side-effects, and get your agreement for your child to receive this treatment. After the planning scan has been performed, the radiation oncologist will construct the treatment plan with the radiotherapy team. During the treatment period, your child will have regular consultations with the radiation oncologist to monitor side-effects. Depending on the centre’s arrangements, the radiation oncologist may be involved in the follow-up visits after treatment.
↑ back to the list
Radiotherapy technologists (RTT) / Therapeutic radiographers
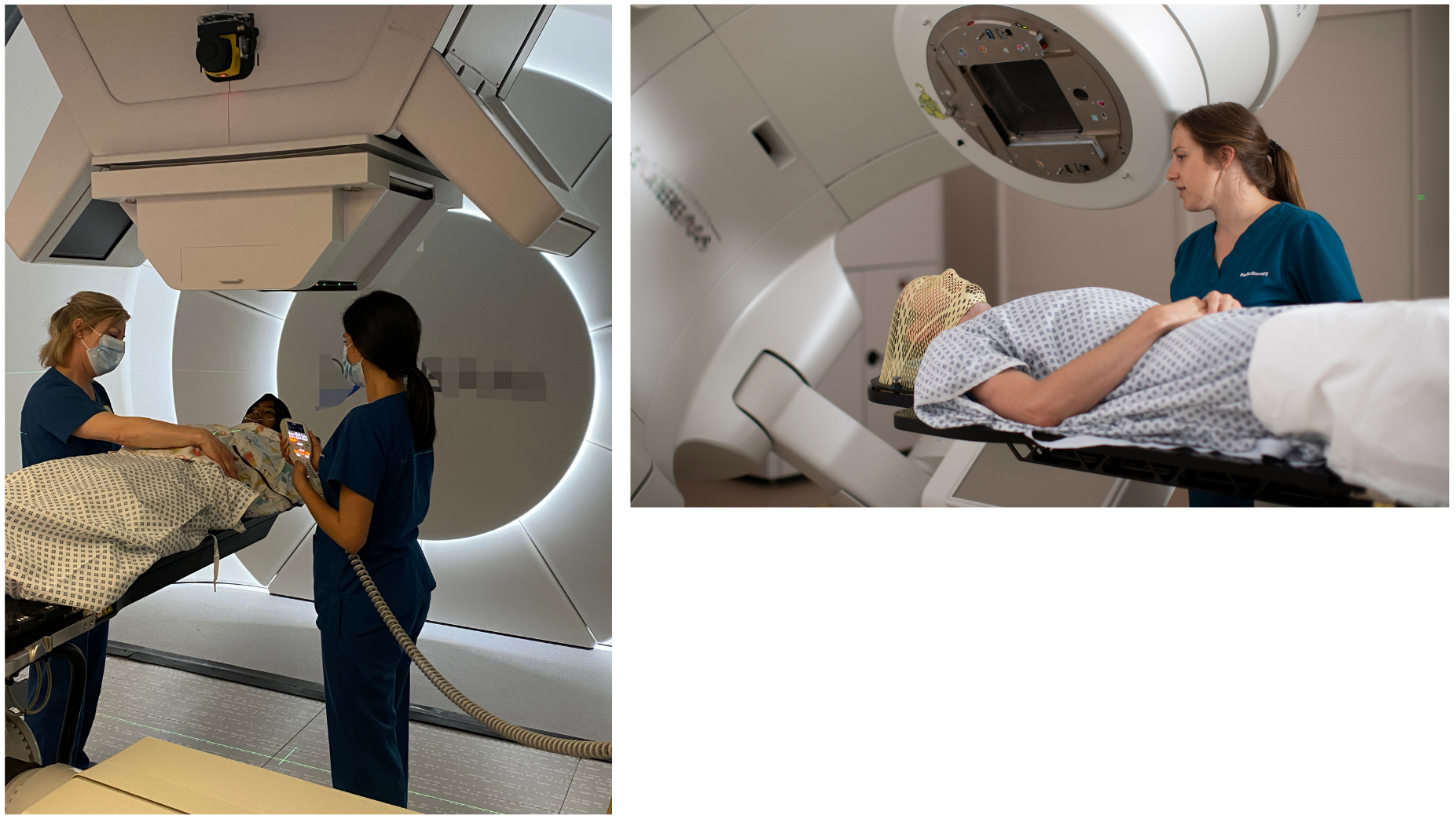
Radiotherapy technologists (RTT), otherwise known as therapeutic radiographers in some countries, are the registered health care professionals responsible for the management of a patient’s radiotherapy treatment pathway, under the supervision of the radiation oncologist. Their responsibilities include the justification of patient specific positioning for treatment, the selection of appropriate immobilisation equipment, the acquisition of the radiotherapy planning scan and utilising technological expertise for accurate treatment delivery.
↑ back to the list
Health Play Specialist
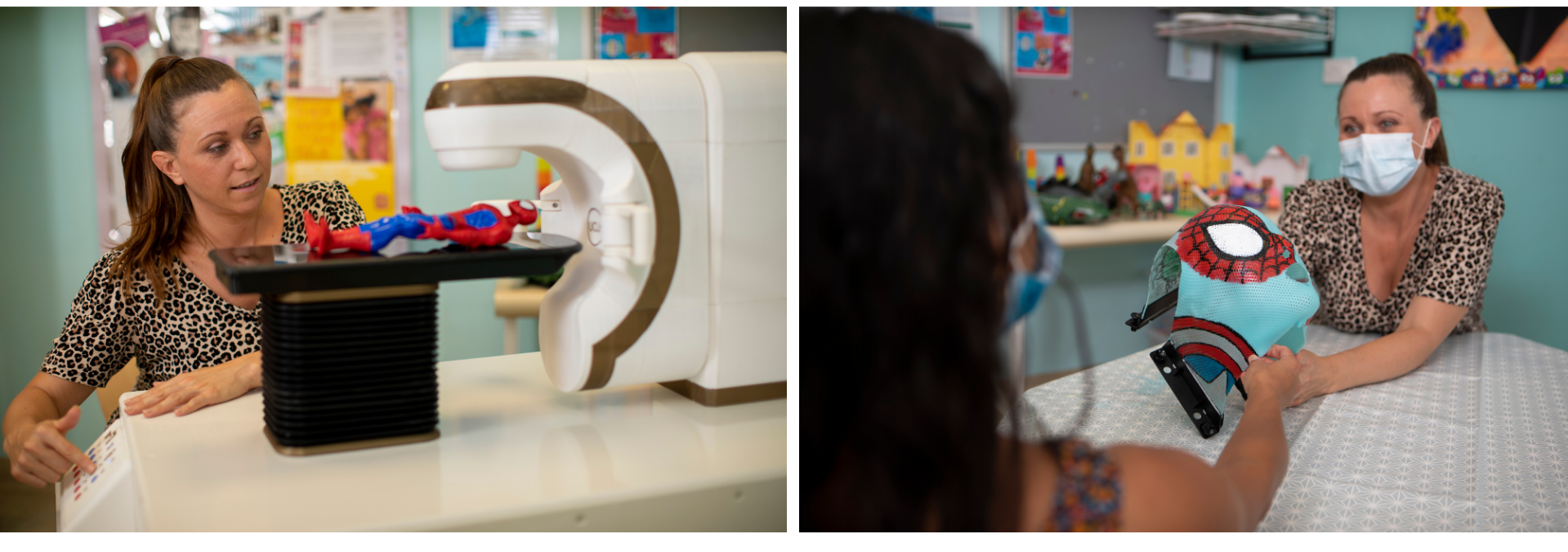
The Health Play Specialists are key team members in the preparation of a child for radiotherapy treatment. Through use of play techniques, videos and demonstrations, the play specialist explains to the child what they can expect throughout the treatment pathway. This is particularly important in helping children to deal with any concerns or feelings they may be having surrounding the treatment.
 Images provided by University College London Hospital
Images provided by University College London Hospital
↑ back to the list
Dosimetrist and Clinical Physicist
Once the patient has had the radiotherapy planning scan, and the radiation oncologist has defined the volume which needs to be treated, the dosimetrist begins to construct an individualised radiotherapy treatment plan. Dosimetrists work directly with the radiation oncologist to design an optimal dose of radiation for treatment. The clinical physicist checks the work of the dosimetrist, using many checks and software programmes to assess the safety of each plan. They are also responsible for making sure the medical equipment and software is used safely. Although patients will rarely meet the dosimetrist and clinical physicist during their treatment pathway, they are key players in the development of a radiotherapy treatment plan.
↑ back to the list
Anesthesiology Team
On the occasion where a child may not be able to remain still for the length of a radiotherapy treatment appointment, especially in younger children, patient sedation may be considered. The anesthesiology team manages the sedation process, working closely with the therapeutic radiographers to carry out the necessary procedures.
↑ back to the list
Other health professionals (e.g. nutritionist, physical therapist)
Depending on the setup of the radiation oncology department or pediatric oncology clinic, you child will have appointments with other health professionals to check-up on specific needs your child might have and to guide them and you during the treatment process. These healthcare professionals can be, for example, nutritionists, physical therapists, psychologists, dentists, social workers etc.
↑ back to the list

